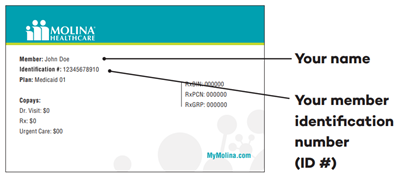
Your Member Identification Card (ID Card)
When you become a member of Molina Healthcare, you get a Molina Member Identification (ID) Card in the mail from us.
Please make sure the information on your Molina Member ID card is right.
- Your name
- Your Molina Healthcare identification number (Identification #)
- Your plan or program name
- Your copays, if applicable
- Additional information on the back of the card:
- Member Services phone number and hours they are open
- Molina Healthcare’s 24-hour Nurse Advice Line toll-free number
- Authorization Department phone number (for your doctor)
- Claims Address (for your doctor)
- Prescription processing information (for your pharmacist)
You may need to show your Molina Member ID Card when you receive physical care of visit the pharmacy.
- Health care providers, such as your doctor, pharmacist and hospital may use your Molina ID card, along with your Utah State Medicaid ID card, to determine if you are eligible for services through Molina Healthcare.
- You can use your paper ID card or get your card electronically through the MyMolina member portal.
- If you lose your Molina Member ID card:
- Go to the MyMolina member portal to access it electronically or to print a temporary Member ID card
- Or you can call Member Services at (888) 483-0760 and ask for a new paper card